Transforming Lives with TMS Therapy
Unlocking the Power of TMS
Find hope and comprehensive treatment with American Psych Care.
What is TMS?
TMS, or Transcranial Magnetic Stimulation, harnesses the potential of non-invasive electromagnetic fields, akin to those generated by an MRI machine, to activate or inhibit specific brain regions. This groundbreaking therapy delivers short, focused magnetic pulses to targeted areas of the brain. The treatment duration varies, ranging from 3 to 19 minutes per session, typically administered 3-5 times per week, spanning a six-week period.




FDA Approved and Insurance Covered
BENEFITS AT A GLANCE
- FDA Approved: Our TMS therapy is backed by the endorsement of the U.S. Food and Drug Administration, ensuring its safety and efficacy.
- No Weight Gain: Unlike some other treatments, TMS therapy won’t lead to unwanted weight gain.
- Insurance Covered: You can access this cutting-edge treatment with the support of your insurance.
Safe and Effective
Minimal Side Effects
- No Sexual Side Effects: TMS therapy boasts a remarkable absence of sexual side effects, enhancing its appeal.
- Safe in Pregnancy: Expecting mothers can rest easy as TMS therapy is considered safe during pregnancy.
- No Memory Side Effects: Preserve your cognitive abilities with TMS therapy, free from memory-related side effects.
Locations
Bel Air
2014 S.Tollgate Rd
Suite 208
Bel Air MD
21015
Silver Spring
11886 Healing Way Suite 504 Silver Spring MD 20904
White Marsh
5009 Honeygo Center Dr Suite 200 Perry Hall MD 21128

TMS Treatment Explained
Experience the Journey
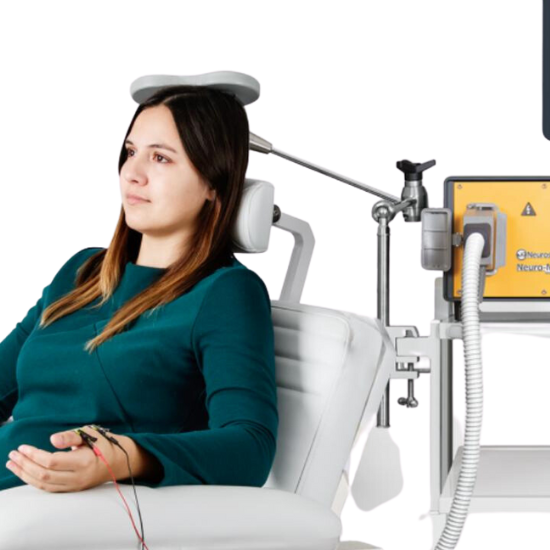
TMS therapy is a painless, noninvasive procedure that requires no anesthesia or sedation. You can continue taking your prescribed medications without interruption. Relax in a comfortable chair, enjoying a spa-like atmosphere, while the TMS coil hovers above your head, delivering the therapeutic magnetic pulses to your brain.
During the treatment, you may hear a clicking noise and feel a gentle tapping sensation on your head, often described as resembling a woodpecker’s sound. Rest assured, TMS treatment is generally pain-free. Following the session, you might experience mild scalp irritation or a minor headache. Each session lasts between 3 to 19 minutes, depending on your treatment plan, allowing you to engage in conversation or watch TV during the process.
Throughout your treatment, our dedicated TMS Therapy specialist remains present, overseeing the procedure and ensuring your comfort.

Treatment Frequency
The Path to Transformation
Most patients undergo three to five TMS treatment sessions per week over a six-week duration. However, the exact frequency can vary based on your specific condition and your response to treatment.
Continuing Medications
Optimizing Your Treatment
You can continue taking your regular medications during your TMS series, but our clinicians will carefully evaluate your medication regimen. In some cases, adjustments may be necessary to mitigate the risk of seizures. Rest assured, our team will work closely with you to optimize your treatment plan.

Long-Term Efficacy
Lasting Relief
TMS offers a durable solution for depression, with responder rates sustained at 50% up to one year following a successful treatment course. While most antidepressant treatments require ongoing maintenance, TMS is no exception. Although research on TMS as a maintenance therapy is limited, our team will collaborate with you and your primary psychiatrist and therapist to establish a maintenance schedule tailored to your needs.
Experience the transformation with TMS therapy. Contact us today to begin your journey toward a brighter future.
Comprehensive Mental Health Services

Child, Adult & Geriatric Psychiatric Clinic:
We are treating children adult and geriatric patients with psychiatric issue.

TMS Brain Stimulation
Center:
FDA approved treatments for conditions like Depression, OCD, fibromyalgia, and chronic insomnia.

Spravato REMS Certified Center:
Specialized care for
Treatment resistant
depression in adults.

Dementia assessment and treatment:
We do Neuro Psych Cognitive assessment test for Dementia - its a comprehensive cognitive function assessment for dementia for psychiatric evaluation

ADHD testing
and treatment:
We provide ADHD testing and treatment services for improved clarity and well-being.

Substance Abuse
Treatment:
Offering treatments like Suboxone,
Vivitrol, Antabuse,
and Acamprosate.

Genetic testing for
psychopharmacology:
Explore personalized psychopharmacology options with our genetic
testing services.

Telemedicine
Services:
Our practice offer tele medicine service based on your insurance coverage. you can see your provider from your mobile phone / ipad/ laptop or computer.

Additional Services:
Psychopharmacology, Brief Psychotherapy, Antipsychotics injection
Meet Our Professionals


Ravikumar Bhalavat


Kathryn Jenkins
What Our Patient Say About Us





